GlytecOne for Health Plans and Value-Based Care Leaders
Diabetes Is Your Largest Controllable Cost Driver. Inpatient Glycemic Data Is the Blind Spot.
As a health plan medical director, ACO leader, or value-based care executive, you are accountable for outcomes and total cost of care across a member population where diabetes is disproportionately represented.
One in four U.S. healthcare dollars is spent caring for people with diagnosed diabetes (Source: Diabetes Care / ADA).
Yet most health plans have limited visibility into what happens to their members’ glucose management during a hospital stay, the care setting where glycemic failures drive the most preventable cost.
Uncontrolled inpatient hyperglycemia and hypoglycemia are associated with longer lengths of stay, higher complication rates, increased readmissions, and avoidable ICU utilization. These costs are absorbed by your plan and attributed to your member outcomes, but they originate in hospital workflows you cannot see and have historically had no way to influence.
GlytecOne’s Population Health solution gives health plan and value-based care leaders the enterprise glycemic intelligence to connect inpatient care performance to longitudinal member health information, identify avoidable cost patterns, and support action.
Why Glycemic Performance Is Now a Health Plan Priority
Three forces are converging to make inpatient glycemic management a strategic concern for every risk-bearing organization.
CMS Is Measuring and Publicly Reporting Glycemic Safety
CMS now requires hospitals to report severe hypoglycemia (NQF #3503e) and severe hyperglycemia (NQF #3533e) as hospital harm eCQMs. These metrics are publicly visible through CMS Hospital Compare and aligned with The Joint Commission’s ORYX program. For health plans evaluating network quality, hospital glycemic performance is becoming a measurable, comparable data point you can use to differentiate high-performing hospital partners from those creating avoidable cost.
Glycemic Failures Drive Disproportionate Downstream Cost
Approximately 40% of non-critically ill hospitalized patients experience hyperglycemia or hypoglycemia (Source: Cleveland Clinic Journal of Medicine). Each severe hypoglycemic event costs an average of $10,000+ in extended care, additional interventions, and liability exposure. When your members experience preventable glycemic harm during a hospital stay, the cost flows through your plan as longer admissions, post-discharge complications, and avoidable readmissions.
Star Ratings, HEDIS, and Risk Adjustment Depend on Glycemic Data
Diabetes-related measures affect CMS Star Ratings, HEDIS performance, and risk adjustment accuracy. Health plans that lack visibility into inpatient glycemic care are missing a significant lever for improving quality scores, closing care gaps at the point of care, and ensuring accurate risk coding for their diabetic member population.
What GlytecOne Population Health Delivers for Health Plans and Value-Based Care Organizations
Population-Level Glycemic Visibility
GlytecOne aggregates glycemic data across hospital partner facilities and care settings into a single population health view. This includes identification of high-cost members through data pattern analysis for structured review, post-discharge data analysis using available inpatient signals, and visibility into which facilities and units are associated with avoidable glycemic-related costs.
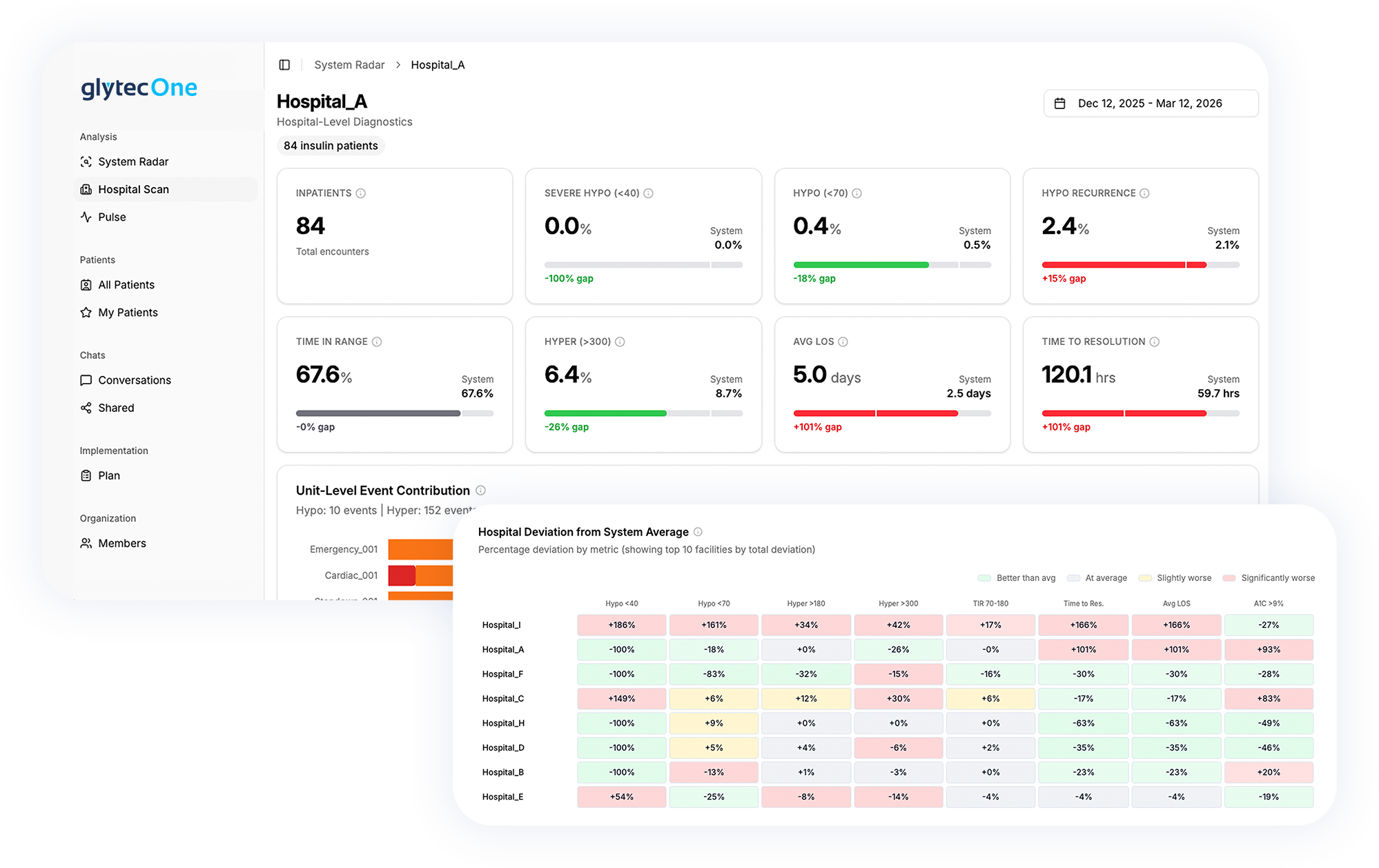
Network Performance Analytics
Compare glycemic performance at the hospital and unit level across your network. Identify facilities associated with avoidable costs through performance analysis. Access performance displays for readmissions, length of stay, pharmacy utilization, gap closure, cost per case, and safety metrics. Analyze care transition flows from hospital to home, skilled nursing facility, and home health settings.
STARS, HEDIS, and Risk Adjustment Support
GlytecOne supports STARS/HEDIS performance and risk adjustment accuracy through open gap detection and closure workflows at point of care, clinical evidence analysis for accurate and timely risk scoring, and audit-ready documentation for defensible coding.
Care Coordination Between Plans and Hospital Partners
Connect inpatient glycemic performance data to longitudinal member health information. Support care coordination workflows between health plans and hospital systems. Give your clinical team the data to identify members who may need post-discharge glycemic intervention before they become readmission statistics.
Built for the Leaders Managing Population-Level Glycemic Risk
Health Plan Chief Medical Officers and Medical Directors
You need to understand which hospital partners are producing glycemic outcomes that affect your member population’s cost and quality trajectory. GlytecOne gives you facility-level and unit-level glycemic performance data so you can identify where preventable harm is occurring and where network interventions can help reduce cost. You also need the data to support STARS/HEDIS performance improvement and risk adjustment accuracy for your diabetic member population. GlytecOne’s open gap detection and clinical evidence analysis help support those goals at the point of inpatient care.
VPs of Population Health and Network Quality
You are responsible for building the analytics infrastructure that connects hospital partner performance to plan-level outcomes. GlytecOne provides the glycemic data layer that most population health platforms lack: inpatient glucose management performance by facility, unit, and care setting, connected to readmission rates, length of stay, cost per case, and care transition patterns. This gives you the evidence base to prioritize network interventions, set performance expectations with hospital partners, and demonstrate glycemic quality improvement across your member population.
The Data Gap You Cannot Afford to Ignore
Most health plans today receive claims data weeks or months after a hospital stay. By then, the preventable glycemic event has already happened. The extended length of stay has already been billed. The readmission is already in progress.
GlytecOne closes that gap by connecting inpatient glycemic care data to your population health infrastructure. Instead of reacting to claims, your team can identify patterns, evaluate network performance, and prioritize interventions based on where glycemic-related costs are concentrated.
Every quarter without population-level glycemic visibility, your organization absorbs avoidable costs that are coded as complications rather than root causes. You miss care gap closure opportunities that affect Star Ratings and risk adjustment accuracy. You lack the data to evaluate hospital partners on glycemic outcomes. And you fall behind competing plans that can demonstrate glycemic quality performance to employers and regulators.
The Numbers That Matter to Your Plan
6–8x ROI
Documented return on investment across GlytecOne partner hospitals
$10,000+
Average cost savings per severe hypoglycemia event avoided
35-68%
Reduction in 30-day readmissions documented by GlytecOne partner hospitals
400+
Hospital partners nationwide in the GlytecOne benchmarking database
99.8%
Reduction in severe inpatient hypoglycemia
1 in 4
U.S. healthcare dollars spent on diagnosed diabetes (Source: ADA)
How Glytec Engages with Health Plan Leaders
Glytec understands that health plan engagement requires a different conversation than hospital procurement. Your priorities are population-level outcomes, network performance, and total cost of care. That is why our engagement model for health plans includes the following.
Population Health Assessment
Glytec’s team works with your analytics staff to map your diabetic member population against available glycemic performance data and identify where avoidable cost is concentrated.
Network Performance Baseline
See how your hospital partners’ glycemic outcomes compare using Glytec’s benchmarking database of 400+ hospitals nationwide.
Custom Financial Modeling
Glytec provides cost modeling tailored to your plan’s member volume, payer mix, and current glycemic-related cost patterns so the value case is built on your numbers.
Transparent Partnership Structure
No hidden costs, no open-ended timelines. Glytec’s Solutions Engineering team manages implementation with your hospital partners, reducing the coordination burden on your team.
See What Glycemic Intelligence Can Do for Your Plan
Book a 30-minute discussion with Glytec’s team. We will walk through how GlytecOne’s Population Health solution connects inpatient glycemic care to the outcomes and costs your plan is already absorbing, and show you what is achievable with enterprise glycemic visibility.
How does inpatient glycemic management affect health plan costs?
Uncontrolled inpatient hyperglycemia and hypoglycemia are associated with longer lengths of stay, higher complication rates, and increased readmissions. Each severe hypoglycemic event costs an average of $10,000+ in extended care and additional interventions. One in four U.S. healthcare dollars is spent caring for people with diagnosed diabetes (Source: Diabetes Care / ADA). Approximately 40% of non-critically ill hospitalized patients experience hyperglycemia or hypoglycemia (Source: Cleveland Clinic Journal of Medicine). For health plans, these costs are absorbed as plan-level spending but originate in hospital glycemic workflows most plans cannot see. GlytecOne’s Population Health solution connects inpatient glycemic performance data to plan-level outcomes, giving health plan leaders the visibility to identify and act on avoidable cost.
What is the connection between hospital glycemic quality and Star Ratings?
Diabetes-related measures affect CMS Star Ratings, HEDIS performance, and risk adjustment accuracy. CMS now requires hospitals to report severe hypoglycemia and severe hyperglycemia as hospital harm eCQMs (NQF #3503e and NQF #3533e). These metrics are publicly visible through CMS Hospital Compare and aligned with The Joint Commission’s ORYX program. Health plans that lack visibility into inpatient glycemic care are missing a lever for improving quality scores and ensuring accurate risk coding. GlytecOne supports STARS/HEDIS performance through open gap detection and closure workflows at point of care, clinical evidence analysis for risk scoring, and audit-ready documentation for defensible coding.
How can health plans reduce diabetes-related hospital costs?
Health plans can reduce diabetes-related hospital costs by gaining visibility into inpatient glycemic management performance across their hospital network. GlytecOne’s Population Health solution aggregates glycemic data across facilities and care settings, enabling identification of high-cost members through data pattern analysis, comparison of facility-level glycemic performance, and analysis of care transition flows. GlytecOne partner hospitals have documented 6-8x ROI and 35-68% reductions in 30-day readmissions. By connecting this hospital-level performance data to plan-level member outcomes, health plans can prioritize network interventions where glycemic-related costs are concentrated.
What are CMS eCQM glycemic safety measures?
CMS requires hospitals to report severe hypoglycemia (NQF #3503e) and severe hyperglycemia (NQF #3533e) as electronic clinical quality measures (eCQMs) under the hospital harm category. The 2026 measurement period is active. Hospitals that do not report risk forfeiting the full 2.6% annual Medicare reimbursement increase. These metrics are publicly visible through CMS Hospital Compare and aligned with The Joint Commission’s ORYX program and Leapfrog Safety Grades. For health plans, these publicly reported measures provide a new, standardized data point for evaluating hospital partner glycemic quality.
How do ACOs manage inpatient diabetes costs?
ACOs are accountable for total cost of care and shared savings performance. Uncontrolled inpatient glycemia is a significant cost driver that most ACOs cannot measure or influence today because glycemic data is fragmented across EHRs and point-of-care devices. GlytecOne’s Population Health solution provides enterprise glycemic intelligence that connects hospital care quality to population health outcomes, giving ACO leaders the data to identify where glycemic-related costs are concentrated and where network improvements can support total cost of care reduction.
What tools help health plans monitor hospital glycemic performance?
GlytecOne’s Population Health solution provides health plans with population-level glycemic analytics across hospital partner networks. Capabilities include network performance analytics that compare glycemic outcomes at the hospital and unit level, performance displays for readmissions, length of stay, pharmacy utilization, gap closure, cost per case, and safety metrics. GlytecOne also supports care transition flow analysis from hospital to home, skilled nursing facility, and home health. The platform aggregates data from GlytecOne’s database of 400+ hospital partners nationwide, providing a benchmarking baseline for network quality evaluation.
How does poor hospital glycemic management increase readmissions?
Poor inpatient glycemic management is associated with glycemic variability that extends lengths of stay, increases complication rates, and creates discharge instability that drives 30-day readmissions. GlytecOne partner hospitals have documented 35-68% reductions in 30-day readmissions through standardized glycemic workflows and FDA-cleared insulin dosing guidance. Clinicians review and confirm all recommendations. For health plans, readmissions driven by glycemic mismanagement represent avoidable plan-level cost that originates in hospital care processes. GlytecOne’s Population Health analytics help plans identify which facilities are associated with higher glycemic-related readmission rates.
What is glycemic population health analytics?
Glycemic population health analytics refers to the aggregation of inpatient glucose management data across multiple facilities and care settings into a unified view that supports enterprise-level decision-making. GlytecOne’s Population Health pillar provides this capability for health systems and health plan partners, including enterprise-wide glycemic performance intelligence, eCQM alignment and value-based care reporting support, health plan partnership tools connecting inpatient performance to longitudinal member health information, and multi-facility benchmarking with site-level performance scorecards.
Schema Markup Recommendation
Implement FAQ schema (application/ld+json) on all eight FAQ items. This supports both Google featured snippet eligibility and AI Overview citation. Each FAQ answer should be self-contained and factually complete without requiring the reader to reference other sections of the page.
Internal Linking Strategy
This page should link internally to the following existing pages: GlytecOne Platform Overview (for visitors who want the full product picture), Population Health pillar page (for deeper technical detail on capabilities), CMS and eCQM Compliance page (for visitors focused on regulatory context), Case Studies page (when payer-relevant case studies become available), and the Financial and Operational Leadership Who We Serve page (for visitors who are also evaluating from a hospital CFO/COO perspective).
Compliance Notes
- All statistics are sourced from approved evidence in Messaging Framework 2.0 and SOP-34 Appendix I
- No payer-specific outcome claims are made (consistent with pilot/early-stage status)
- Hospital-side proof points (6-8x ROI, 35-68% readmission reduction, $10K+ per event) are attributed to GlytecOne partner hospitals, not to health plan outcomes
- Glucommander referenced as FDA-cleared Class II SaMD with ‘clinicians review and confirm all recommendations’ included where dosing is described
- Command Center capabilities described using approved language: ‘current and historical performance data’ per SOP-34 guidance
- No AI, machine learning, or predictive language used per SOP-34 automatic escalation triggers
- No use of FDA logo or visual elements suggesting FDA endorsement
- Language uses ‘supports,’ ‘helps,’ ‘can help,’ and ‘associated with’ framing per Messaging Framework tone guidelines
- CTA follows approved pattern: ‘Book a [context] Discussion’ as primary; content download as secondary
Content Gap: Future Additions
As payer partnerships mature beyond pilot stage, this page should be updated to include named health plan partner references (with approval), payer-specific ROI case studies, Star Rating or HEDIS improvement data tied to glycemic management, and testimonial quotes from health plan medical directors or population health executives. Until then, all proof points remain hospital-side with logical connection to plan-level implications.
Recommended Next Steps
- Review this deliverable with clinical, marketing, and regulatory stakeholders for SOP-34 compliance sign-off
- Add the page to the Who We Serve navigation between ‘Providers and Nurses’ and ‘Financial and Operational Leadership’ (or at the end, after Financial and Operational Leadership)
- Implement FAQ schema markup for AEO optimization
- Create a corresponding ‘Population Health Overview’ downloadable PDF or one-pager for the secondary CTA
- Brief the sales team on the payer-facing engagement model described in the ‘How Glytec Engages’ section
- Set up keyword tracking for all primary and long-tail SEO terms in your preferred rank tracking tool